Alex's story
It was an eventful day on Friday. I had my last OB appointment and non-stress test at 10.15. (I was scheduled to be induced on the the 28th.) The baby didn't cooperate on the NST so after an hour, I saw the doctor and then went to Radiology for another bio-physical ultrasound. That's where they measure the amniotic fluid, count gross and fine movements, check the heart rate and watch the breathing. The baby had failed twice before so I knew what was going on and wasn't too worried. Both times we were cleared immediately and sent home. This time, however, the tech was unable to observe 30 seconds of continuous breathing. After the Radiologist reviewed the scan and talked to my doctor, I had to go back to her office. I called Neil as I walked back over and told him to be ready to get the next train. Sure enough, that was confirmed as soon as I saw my doctor.
One of my favorite nurses walked me over to Labor and Delivery and the adventure continued. I was admitted and taken into a room. I didn't realize till later that it wasn't an actual delivery room. After almost an hour a nurse came in to tell me that they were actually full! There was one open delivery room, but they wanted to keep that open for an emergency walk-in. She wanted to know if I objected to starting the induction in that room and then going into another room as one opened. I said I didn't, but once she heard how fast I usually go, they decided to wait till I was in a delivery room to start the pitocin.
Neil arrived about 4.15 and I was finally moved around 5.30. They started the pitocin at 5.55 and the doctor broke my water at 6.05. Contractions started pretty quickly after that. I had an awesome nurse and she kept telling me to get the epidural as soon as I felt contractions so by 7.30, I was getting the epidural. We had warned the nurses and anesthesiologist that after both of my previous epidurals my BP crashed and I had to have a dose of epinephrine to raise it back up. This anesthesiologist was truly the best one I've ever met. He went really slowly, he waited for me to get through a contraction and he was very personable. He gave me a lower dose so I didn't crash immediately. Soon, I was feeling great.
A few minutes later, I started feeling kind of strange. When I finally said something to Neil, I was really out of it. I felt totally lucid, but apparently I wasn't. I remember that I was having a hard time breathing and was slurring my words. He called the nurse in and she immediately pushed the call button to get the anesthesiologist. Then she had Neil pull the code button in the room to get him there faster. She said we couldn't wait for the nurse's station. I can remember this happening, but it was like watching a movie rather than happening to me. The doctor came running and he gave me a dose of epinephrine and lowered the dose of epidural. I was soon back to normal.
This happened four more times. I don't even remember two of the episodes. I'm still learning details from Neil. My BP dropped to 50/43. The nurse told him I almost ended up in the OR twice. I may have thought I was lucid, but I was "gone" according to him. The anesthesiologist was paged for every episode. At one point he stopped in to check on me and showed me a syringe of epinephrine. He said he never did this, but he was walking around with it in his pocket waiting for the next page. Once we finally got the dose of epinephrine and epidural balanced, I was nearly ready to push.
Another lovely side effect is they pumped me full of saline to help raise my BP. I had over 2 liters put in and nothing was coming out. The nurse promised I'd swell up and go home weighing more than I when I came in because of the swelling. Wow, was she right!
Once I was ready to push, things moved very quickly. Three pushes and his head was out. Dr. Anderson said not to push and I assumed that she was just suctioning his mouth out. I didn't know till later that the cord was wrapped around his neck 5 times--a new hospital record! She slipped her finger under the cord, clamped and cut it immediately. One final push and he was out and then they told me about the cord around his neck. I panicked so it's probably a good thing they waited to tell me. Neil said he wasn't that worried because he could see that
Alex wasn't blue.
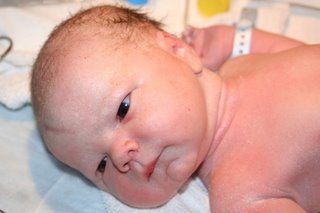 Of course, we didn't know what we were having so all of this drama was over by the time we found out we had another son! We weren't certain of his name before, but Neil said he looked like an Alexander so we went with our original choice. William is Neil's Dad and Grandad so we continued our tradition of naming after loved ones.
Of course, we didn't know what we were having so all of this drama was over by the time we found out we had another son! We weren't certain of his name before, but Neil said he looked like an Alexander so we went with our original choice. William is Neil's Dad and Grandad so we continued our tradition of naming after loved ones.
Because Alex was large for his gestational age, they had to check his blood sugar right away. He wasn't able to maintain it at an acceptable level, so they took him to the NICU a few hours after he was born. He was on a sugar water IV to keep his levels up. Every baby that goes to the NICU is put on broad-spectrum antibiotics while they culture blood samples to check for infection. It takes about 48 hours for the cultures so he spent 2 days in the NICU while I was in my room. We were able to go see him whenever we wanted. I was able to get up in the night and go hold him for awhile if I wanted. I think I only missed 1 feeding while we were in the hospital. My mom was able to go in for a visit, but unfortunately, Emma and Andy weren't allowed in the NICU. It's RSV season so no children are allowed. We were able to unhook him from the monitors and take him to a window so the kids could at least see him yesterday. It wasn't the meeting that we had planned for, but it was still special to watch them see Alex for the first time.
When the neonatologist heard that I was going home today, he checked Alex and said he didn't see why he couldn't go home with me after his last dose of antibiotics at 4 pm. We expected him to have to stay till Monday so we were all very happy!
I have pictures of Alex's homecomming, but for some reason can't get them to load. I'll keep trying and will post an update when I do.
One of my favorite nurses walked me over to Labor and Delivery and the adventure continued. I was admitted and taken into a room. I didn't realize till later that it wasn't an actual delivery room. After almost an hour a nurse came in to tell me that they were actually full! There was one open delivery room, but they wanted to keep that open for an emergency walk-in. She wanted to know if I objected to starting the induction in that room and then going into another room as one opened. I said I didn't, but once she heard how fast I usually go, they decided to wait till I was in a delivery room to start the pitocin.
Neil arrived about 4.15 and I was finally moved around 5.30. They started the pitocin at 5.55 and the doctor broke my water at 6.05. Contractions started pretty quickly after that. I had an awesome nurse and she kept telling me to get the epidural as soon as I felt contractions so by 7.30, I was getting the epidural. We had warned the nurses and anesthesiologist that after both of my previous epidurals my BP crashed and I had to have a dose of epinephrine to raise it back up. This anesthesiologist was truly the best one I've ever met. He went really slowly, he waited for me to get through a contraction and he was very personable. He gave me a lower dose so I didn't crash immediately. Soon, I was feeling great.
A few minutes later, I started feeling kind of strange. When I finally said something to Neil, I was really out of it. I felt totally lucid, but apparently I wasn't. I remember that I was having a hard time breathing and was slurring my words. He called the nurse in and she immediately pushed the call button to get the anesthesiologist. Then she had Neil pull the code button in the room to get him there faster. She said we couldn't wait for the nurse's station. I can remember this happening, but it was like watching a movie rather than happening to me. The doctor came running and he gave me a dose of epinephrine and lowered the dose of epidural. I was soon back to normal.
This happened four more times. I don't even remember two of the episodes. I'm still learning details from Neil. My BP dropped to 50/43. The nurse told him I almost ended up in the OR twice. I may have thought I was lucid, but I was "gone" according to him. The anesthesiologist was paged for every episode. At one point he stopped in to check on me and showed me a syringe of epinephrine. He said he never did this, but he was walking around with it in his pocket waiting for the next page. Once we finally got the dose of epinephrine and epidural balanced, I was nearly ready to push.
Another lovely side effect is they pumped me full of saline to help raise my BP. I had over 2 liters put in and nothing was coming out. The nurse promised I'd swell up and go home weighing more than I when I came in because of the swelling. Wow, was she right!
Once I was ready to push, things moved very quickly. Three pushes and his head was out. Dr. Anderson said not to push and I assumed that she was just suctioning his mouth out. I didn't know till later that the cord was wrapped around his neck 5 times--a new hospital record! She slipped her finger under the cord, clamped and cut it immediately. One final push and he was out and then they told me about the cord around his neck. I panicked so it's probably a good thing they waited to tell me. Neil said he wasn't that worried because he could see that
Alex wasn't blue.
 Of course, we didn't know what we were having so all of this drama was over by the time we found out we had another son! We weren't certain of his name before, but Neil said he looked like an Alexander so we went with our original choice. William is Neil's Dad and Grandad so we continued our tradition of naming after loved ones.
Of course, we didn't know what we were having so all of this drama was over by the time we found out we had another son! We weren't certain of his name before, but Neil said he looked like an Alexander so we went with our original choice. William is Neil's Dad and Grandad so we continued our tradition of naming after loved ones.Because Alex was large for his gestational age, they had to check his blood sugar right away. He wasn't able to maintain it at an acceptable level, so they took him to the NICU a few hours after he was born. He was on a sugar water IV to keep his levels up. Every baby that goes to the NICU is put on broad-spectrum antibiotics while they culture blood samples to check for infection. It takes about 48 hours for the cultures so he spent 2 days in the NICU while I was in my room. We were able to go see him whenever we wanted. I was able to get up in the night and go hold him for awhile if I wanted. I think I only missed 1 feeding while we were in the hospital. My mom was able to go in for a visit, but unfortunately, Emma and Andy weren't allowed in the NICU. It's RSV season so no children are allowed. We were able to unhook him from the monitors and take him to a window so the kids could at least see him yesterday. It wasn't the meeting that we had planned for, but it was still special to watch them see Alex for the first time.
When the neonatologist heard that I was going home today, he checked Alex and said he didn't see why he couldn't go home with me after his last dose of antibiotics at 4 pm. We expected him to have to stay till Monday so we were all very happy!
I have pictures of Alex's homecomming, but for some reason can't get them to load. I'll keep trying and will post an update when I do.

0 Comments:
Post a Comment
<< Home